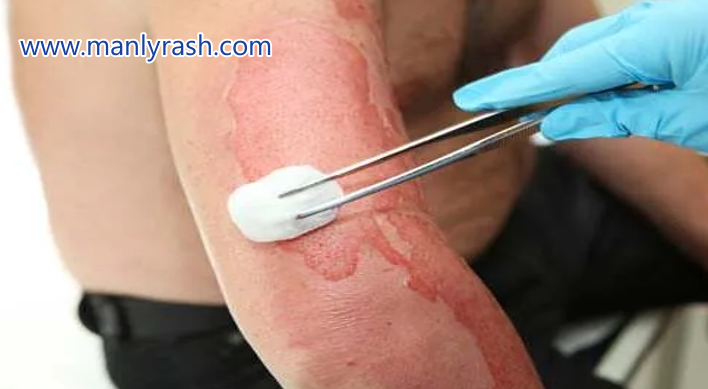
Improper treatment can lead to various long-term complications including wound infection.
If you don’t treat cuts properly, they can get infections and other problems in the future. When dangerous germs or bacteria enter the body through an open wound, infections can occur. Untreated or poorly managed diseases can lead to numerous complications. Problems that can happen include wounds that don’t heal properly, abscesses, tissue damage, infection spreading, and the growth of new illnesses. To avoid or lower the risk of long-term problems from wound infections, it is important to take care of wounds properly and act quickly.
Read More
When a wound occurs on the body, severe pain can be experienced. In addition, the following conditions may develop at the site of the wound:
– Redness of the skin.
– Formation of blisters.
– Swelling.
– Discharge or oozing.
– Darkening or whitening of the skin around the wound.
– Formation of a scab.
It is important to note that even though severe pain may not always accompany a wound, deep wounds can damage nerves, leading to loss of sensation. Therefore, it is advisable to seek prompt medical attention in such cases.
Apart from high temperature, the body can experience burns due to various other causes, such as electrical shock, radiation, severe friction, and contact with corrosive acids or chemicals. The term "burns" commonly refers to these types of injuries, distinct from regular wounds. The treatment methods for these burns also differ from those of ordinary wounds.
Primary Treatment for Burns
High temperature can cause two types of burns—dry heat burns and wet heat burns. Dry heat sources include fire, hot objects, and hot metals, while wet heat sources include hot water and steam. However, the initial treatment for both types of burns remains the same.
It is crucial to initiate primary treatment for burns as quickly as possible, regardless of the type of burn. This helps minimize damage to the skin. Follow the steps below for primary treatment of burns:
1. Move away from the heat source
Quickly move the affected person away from the source of heat. If anyone is nearby, call for help or assistance.
2. Extinguish the flame on clothing
To extinguish flames on clothing, use a heavy blanket, roll the person on the ground, or use a fire extinguisher. You can also smother the flames with water or use a fire suppression device. If their clothes catch fire, help them remove the clothing immediately.
3. Cool with abundant water
For cooling the affected area, place it under cool running water for at least 20 minutes. If running water is not available, use a container or a showerhead to pour cool water over the burn. Avoid using ice or very cold water as it may further damage the skin.
It is important to note that using water at normal temperature or slightly cool water is recommended. Do not use ice or extremely cold water.
4. Remove clothing and fabrics
Remove clothing and fabrics from the affected area. However, if anything is stuck to the skin, do not forcefully remove it.
5. Cover the burn
Cover the burn with a clean, sterile dressing. If a sterile dressing is not available, you can use clean, non-stick fabric or plastic wrap as a temporary solution.
6. Keep the body wrapped in a cloth
Wrap the person in a clean blanket or sheet to maintain an optimal body temperature. Ensure that there is no pressure or tightness on the affected area and take care to avoid friction.
Note:
Seeking immediate medical attention is crucial for severe burns or burns that involve the face, hands, feet, genitals, or major joints. A healthcare professional will provide appropriate medical advice and further guidance.
7. Take pain relievers
For pain relief, you can take over-the-counter pain medications such as paracetamol or ibuprofen.
8. Keep the patient seated
If the mouth or eyes are affected, try to keep the patient seated. This position can help reduce swelling. On the other hand, if the feet or lower body are affected, elevate the legs and keep the patient lying down.
9. Rinse chemical burns
Carefully remove any soaked clothing contaminated with chemicals. Rinse the affected area with a copious amount of water until you can seek medical attention.
Read more
14 Essentials of Diabetes Control
What should not to do
1. Avoid attempting extensive wound treatment at home.
2. Toothpaste, oil, and turmeric should not be applied to the wound.
3. Do not apply ice or extremely cold water to the wound. This can further deepen the injury.
4. Do not pour or splash cold water on the patient’s body for an extended period. This can lead to excessive chilling of the body.
5. Do not directly apply forceps, tissue, or cream to the wound.
6. Do not attempt to stitch the wound before reaching the hospital.
7. Dressing the wound or applying any antiseptic or ointment without a doctor’s advice is not recommended.
8. Refrain from providing primary medical treatment to others without ensuring your own safety.
After providing initial first aid, whether or not to take the patient to the hospital will depend on the type and severity of the burn, as well as various factors. Here are some considerations:
Burn type:
Different types of burns may require medical attention. For example, chemical burns, electrical burns, or deep burns should be evaluated by a healthcare professional.
Burn severity:
Burns are classified into degrees based on their severity. First-degree burns generally do not require hospitalization, while second-degree burns may need medical assessment. Third-degree burns, which are the most severe, almost always require immediate medical attention.
Burn size and location:
Burns covering a large area of the body or those located on critical areas such as the face, hands, feet, genitals, or major joints may require hospital evaluation.
Age and health condition:
Infants, young children, the elderly, and individuals with pre-existing medical conditions might be more susceptible to complications from burns. Hospitalization may be necessary in these cases.
Signs of infection:
If signs of infection develop, such as increasing pain, redness, swelling, pus, or fever, medical attention should be sought promptly.
Inhalation injury:
If the burn occurred due to inhalation of smoke or chemicals, the patient should be taken to the hospital for evaluation, as airway and respiratory complications can arise.
Tetanus vaccination status:
If the patient’s tetanus immunization is not up to date, a healthcare professional should assess the need for a tetanus shot.
It is important to consult a healthcare professional for a proper evaluation and guidance on whether hospitalization or further medical intervention is necessary based on the specific circumstances of the burn.
When to visit a doctor:
If the burn is severe, it is advisable to take the patient to a doctor. If possible, consider visiting a specialized hospital for burn and plastic surgery, such as the Sheikh Hasina National Institute of Burn and Plastic Surgery, or a nearby major hospital with a burn unit.
In such specialized facilities, the medical professionals have expertise in treating burns and can provide the necessary care and treatment for severe burns. They have the resources and equipment required to handle complicated burn cases.
In the following four situations, the burn patient should be taken to the hospital without delay:
1.Large or deep burns:
If the burn is larger in size or deep compared to the palm of the person’s hand.
2.Involvement of critical areas:
If the burn affects special areas such as the hands, feet, eyes, face, genitalia, or if the burn covers a significant portion of these areas.
3.Skin turning white or black:
If the skin at the burn site turns white or black, regardless of the extent.
4.Chemical or electrical exposure:
If the burn occurred due to chemical or electrical exposure to the body.
In the case of burns, there is a higher risk of complications in women, elderly individuals, and children under five years of age. Therefore, it is advisable to consult a doctor for any type of burn in these populations.
If there is inhalation of hot smoke or fumes, it is important to seek medical advice. Symptoms such as coughing, throat pain, or difficulty breathing may take some time to manifest. Therefore, it is not advisable to neglect these symptoms.
It is crucial to prioritize the well-being and safety of individuals in these vulnerable groups and seek prompt medical attention for burns.
Vital Information:
In some cases, severely burned patients may experience a life-threatening condition called “shock,” where the body’s oxygen supply can significantly decrease. This can have serious implications for the patient’s life. In this condition, the following symptoms may be observed:
1. Coolness of the body due to decreased body temperature.
2. Increased heart rate or pulse. It is important to note that the average resting pulse rate for adults is between 60-100 beats per minute.
3. Rapid and shallow breathing.
4. Pale or clammy appearance of the face.
5. High or persistent low blood pressure.
6. Confusion or loss of consciousness.
If these symptoms are observed, it is essential to immediately transport the patient to the nearest hospital for appropriate medical care.
Please note that this information is provided as general guidance, and it is crucial to consult with a healthcare professional for accurate diagnosis and personalized treatment based on the specific circumstances of the burn patient.
Before reaching the hospital, please perform the following three actions:
1. If possible, lay the patient down on a flat surface and elevate their legs, keeping them slightly elevated. You can provide a pillow or cushion under the patient’s legs if available.
2. Cover the patient’s body with a clean blanket or sheet, excluding the burned areas. This will help maintain body temperature and prevent further contamination.
3. Refrain from giving the patient any food or drink orally. Inhaling or ingesting anything can potentially lead to infection in the respiratory system and pose a risk to the patient’s life.
Please remember that these actions should be taken while prioritizing the safety and well-being of the burn patient. It is crucial to seek immediate medical attention and follow the guidance of healthcare professionals for proper evaluation and treatment.
Medical Treatment at the Hospital:
In the hospital, the extent of the burn injury will be assessed, and specific protocols will be followed accordingly. The severity of the injury will be evaluated, and the wound will be cleaned and dressed appropriately.
In cases of severe burns, it may be necessary to perform surgery for skin grafting or other procedures to replace damaged skin. This helps in promoting healing and preventing complications such as fluid loss and infection. Additionally, various medications, including saline solutions, may be administered to address dehydration and other complexities caused by the burn.
It is important to note that burn treatment requires specialized care, and healthcare professionals will determine the most suitable course of action based on the individual patient’s condition.
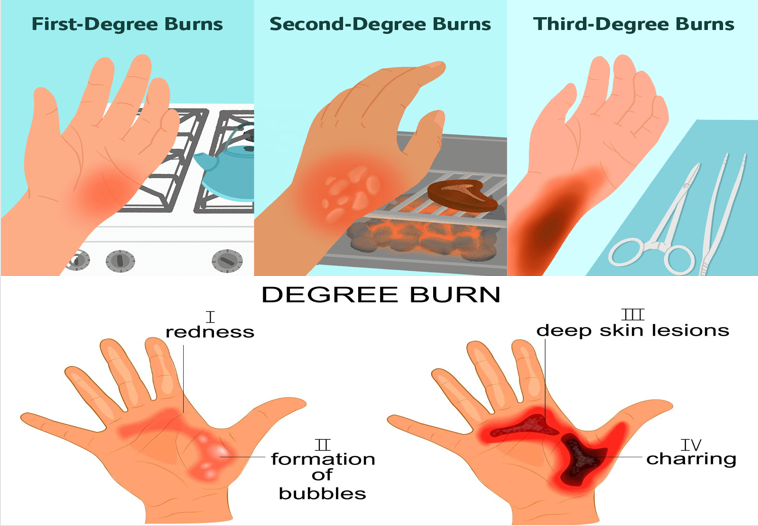
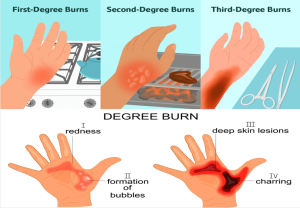
Types of Burns:
Burns can be classified based on the depth of skin involvement and the layers of the skin affected. Our skin has three main layers, which are:
1. Epidermis:
This is the outermost layer of the skin. It provides a protective barrier against the environment. Superficial burns that only affect the epidermis are called superficial or first-degree burns. They typically result in redness, pain, and mild swelling, such as sunburns.
2. Dermis:
The dermis is located just beneath the epidermis and consists of tissues that include blood vessels, nerves, sweat glands, hair follicles, and sebaceous glands. Burns that extend into the dermis are categorized as partial-thickness or second-degree burns. These burns can cause blistering, intense pain, and redness.
– Superficial partial-thickness burns: These burns affect the upper layers of the dermis and appear as moist, pink, and blistered areas.
– Deep partial-thickness burns: These burns extend deeper into the dermis and may appear white or mottled. They are often less painful than superficial partial-thickness burns.
3. Subcutis (also known as subcutaneous tissue):
The subcutis is the deepest layer of the skin and consists of fat cells, blood vessels, and connective tissue. Burns that reach the subcutis are considered full-thickness or third-degree burns. The affected area may appear charred, white, or leathery. Full-thickness burns typically result in numbness because the nerve endings are destroyed.
Additionally, there is a fourth-degree burn, which extends beyond the skin and affects the underlying muscles, tendons, ligaments, or bones.
The depth of the burn injury determines the severity and potential complications associated with the burn. Proper assessment and classification of burns are crucial for determining appropriate treatment plans and interventions.
First-Degree Burn:
A first-degree burn affects the epidermis, the outer layer of the skin, and is caused by exposure to heat. The affected area turns red and may experience mild pain and swelling. A common example of a first-degree burn is sunburn, where the skin becomes red but does not blister.
In the case of a first-degree burn, basic first aid measures such as applying cool water or a cold compress can be used. Medical attention is generally not required for this type of burn, although it is advisable to consult a healthcare professional for guidance.
It is important to exercise caution and follow the recommendations of healthcare professionals to accurately identify the type and severity of a burn and to ensure appropriate treatment.
Second-Degree Burn:
A second-degree burn affects both the epidermis and the dermis, which are the outer and underlying layers of the skin, respectively. The affected area will appear pink or red and may develop blisters. The pain experienced with a second-degree burn can be more intense compared to a first-degree burn.
In the case of a second-degree burn, the affected area may exhibit a mottled appearance with pink or red patches and blister formation. The blisters can vary in size and may be filled with clear fluid. The burn site may also be painful and sensitive to touch.
When providing first aid for a second-degree burn, it is important to cool the burn with cool water, but not ice, and cover it with a clean, non-stick dressing. Seek medical attention for proper assessment and treatment, as some second-degree burns may require professional care, such as cleaning, dressing changes, and potential topical treatments or antibiotics to prevent infection.
It is essential to consult a healthcare professional for an accurate diagnosis and appropriate management of second-degree burns, as they can vary in severity depending on the extent and depth of the burn.
Third-Degree Burn:
A third-degree burn is the most severe type of burn and affects both the epidermis and dermis layers of the skin. The affected area appears red or mottled, and the skin may be charred, white, or leathery in texture. Third-degree burns can result in the destruction of nerve endings, leading to a lack of sensation in the burned area.
In the case of a third-degree burn, the skin may be dry or moist, depending on the extent of the burn and associated injury. The burn site may have a patchy, waxy, or translucent appearance. Additionally, there may be areas of eschar (black or brown dead tissue) present. Third-degree burns are typically not painful initially due to nerve damage, although surrounding areas may experience pain.
Third-degree burns require immediate medical attention. These burns often necessitate specialized burn care, such as wound cleaning, debridement (removal of dead tissue), and various treatments like skin grafting. Infections are a significant concern with third-degree burns, so antibiotics and proper wound care are crucial to prevent complications.
It is essential to seek emergency medical care for third-degree burns, as they can pose significant health risks and may require extensive treatment and rehabilitation.
Fourth-Degree Burn:
A fourth-degree burn is an extremely severe type of burn that affects all layers of the skin, including the epidermis, dermis, and subcutaneous tissue. In this type of burn, the entire thickness of the skin is destroyed, and the underlying tissues, such as muscles, tendons, and bones, may also be involved. The burned area may appear charred or blackened.
The skin underneath the burn may have a waxy or leathery texture and can be dry or appear moist. The remaining skin around the burn site may appear dry and pale, reddish-brown, or black. Unlike lower-degree burns, fourth-degree burns are often not painful due to the extensive nerve damage. However, there may be pain in the surrounding areas.
Fourth-degree burns are life-threatening and require immediate medical attention. Emergency medical care is essential for these burns, as they can result in severe complications, including infection, loss of function, and systemic effects. Treatment may involve surgical interventions, such as excision of the burned tissue, skin grafting, and intensive wound care.
It is crucial to seek immediate medical help if a fourth-degree burn is suspected, as specialized medical care is necessary to manage and treat this type of burn effectively.
Ways to Prevent Fires and Burns
Taking precautionary measures at home can significantly reduce the risk of fire and burn accidents. Follow these guidelines:
1. Use of Non-Conductive Materials
– Never touch electrical appliances or conductive materials with wet hands.
– Avoid using exposed electrical lines carelessly.
2. Home Safety Measures
– Regularly inspect and maintain the electrical and gas lines in your house. Promptly address any issues.
– Keep the water temperature low in bathrooms with geysers or hot water lines.
– Refrain from smoking and using other fire sources inside your house.
3. Cooking Safety Precautions
– Develop a habit of always turning off the stove after cooking.
– Take caution with clothing worn while cooking (e.g., sarees, veils, or towels). Consider wearing a fire-retardant apron if available.
– Handle hot water and other hot objects with care.
4. Special Precautions for Children
– Keep young children away from the kitchen and sources of flames (e.g., lighters, matches, candles) as well as hot beverages like tea and coffee.
– Test the water temperature before bathing children, using your elbow to gauge its heat.
5. Enhanced Safety at Home and Work
– Install smoke alarms and ensure emergency staircases for quick evacuation in case of fire.
– Keep fire extinguishers on every floor of the building, accompanied by written instructions on how to use them. Consider coordinating this provision with all tenants in the building.
– Clearly display the phone number of the fire service in a visible location.
By implementing these fire prevention measures, you can greatly reduce the risk of fire incidents and protect yourself, your family, and your property from potential harm.
Written By Dr Senjuti Seemanta
Medical review done by Dr. Ima Islam
Most Important Post For You

Is the baby gaining weight?
Health-conscious people think about their weight as they age. Weight considerations also work for some of the younger generations. But children are different. How much

The Importance of Breastfeeding: Why Formula Milk Falls Short
Introduction: Breastfeeding is a vital aspect of infant nutrition, providing numerous health benefits for both babies and mothers. Exclusive Breastfeeding (EBF) during the first six

Are you using the inhaler correctly?
Inhalers are a common treatment for respiratory diseases. It is very effective for lung problems like asthma and COPD. Salbutamol, an inhaler-delivered steroid-like medicine, effectively

Responses to frequently asked questions on diabetes
What is the home remedy for diabetes? How much diabetes is normal after eating on an empty stomach? This article presents answers to all common

What are the symptoms of diabetes?
Many people are unknowingly suffering from type 2 diabetes due to not knowing the symptoms. Doctors often diagnose diabetes when they perform a blood or

What to do if diagnosed with type 2 diabetes?
By making some changes in their daily lives, many people can live a healthy life by keeping diabetes under control. However, it is important to
Hyperglycemia or Increased Sugar
Increased blood sugar, or blood sugar level, is called hyperglycemia. This is a known problem for diabetic patients. Hyperglycemia can occur in patients with any

Diabetic Food List
If you need to change your diet, try making small changes each week. A healthy diet will help keep your diabetes under control. At the
What to do if burned
Improper treatment can lead to various long-term complications including wound infection. If you don’t treat cuts properly, they can get infections and other problems in
What is the way to eliminate gastric?
Gastric problems happen to more or less everyone. If you know how to remove the gastric, you can get rid of this problem. Gastric symptoms

5 Strategies to Prevent Diabetes
Healthcare professionals first advise individuals with diabetes to avoid consuming sugary or sweet foods. And this is exactly why there is a common belief that

You don’t have to give up sugar, pay attention to 3 habits to stay diabetes free
Blood sugar levels are high. Many favorite foods had to be eliminated from the diet. From tea to chutney, sugar has been removed from all